This website uses cookies so that we can provide you with the best user experience possible. Cookie information is stored in your browser and performs functions such as recognising you when you return to our website and helping our team to understand which sections of the website you find most interesting and useful.
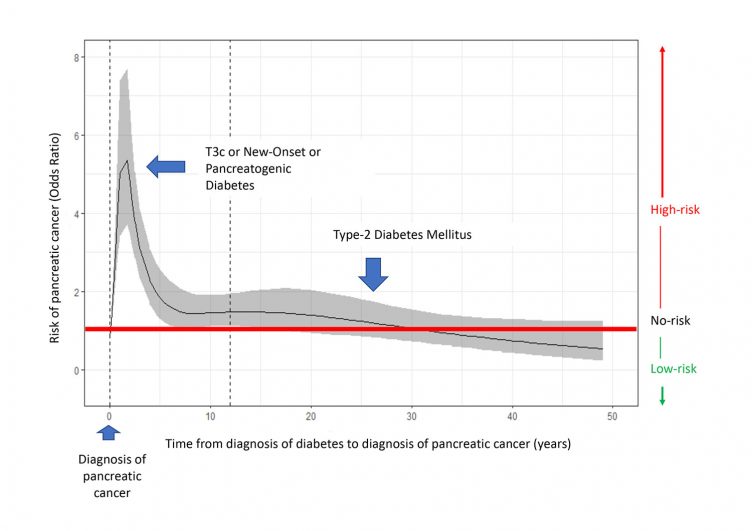 Nonlinear association between the risk of pancreatic cancer and the time elapsed between the diagnosis of diabetes and that of pancreatic cancer. Point 0 represents the diagnosis of pancreatic cancer. Diagnosis of diabetes less than 2 years before cancer diagnosis is strongly associated with the risk of this tumour. /CNIO
Nonlinear association between the risk of pancreatic cancer and the time elapsed between the diagnosis of diabetes and that of pancreatic cancer. Point 0 represents the diagnosis of pancreatic cancer. Diagnosis of diabetes less than 2 years before cancer diagnosis is strongly associated with the risk of this tumour. /CNIO
The high mortality of pancreatic cancer is a consequence of late diagnosis because of the absence of symptoms in the earliest stages, and defining risk populations is therefore crucial to be able to carry out diagnostic tests that reveal the presence of the tumour as early as possible
The CNIO team of researchers confirms that a high percentage of cases of diabetes type 3c is caused by this type of cancer; this finding should prompt further research to allow these patients to enter in early pancreatic cancer diagnosis interventions to increase their survival rate
The team used data from more than 3,500 persons from PanGenEU, a large European study led by the researchers themselves, involving centres from six countries, including Spain, to analyse the relationship between multiple risk factors and pancreatic cancer
As biomedical sciences incorporate increasingly sophisticated methodologies and technologies, our understanding of diseases improves. Diabetes is a clear example since new classifications are being added to the traditional classification into type 1 and type 2 diabetes; these new classifications are based on genetic and molecular characteristics that improve diagnosis and treatment.
The Genetic and Molecular Epidemiology Group, led by Núria Malats at the Spanish National Cancer Research Centre (CNIO), shows the need to continue to improve these classifications: the team published in the journal Gut the results of a European case-control study showing that one of the most recently identified types of diabetes, type 3c or pancreatogenic diabetes, could also be an early manifestation of pancreatic cancer.
This type of cancer has a high mortality rate – around 95% – since it is usually diagnosed too late because of the absence of symptoms in its early stages. Therefore, the finding of the CNIO would imply that it is possible to make an earlier diagnosis of this disease since it allows classifying patients with diabetes type 3c as a population with an increased probability of having early stage pancreatic cancer.
A camouflaged symptom
Diabetes and pancreatic cancer are connected because the pancreas secretes insulin; in diabetic people, this does not occur in a normal way. It is estimated that around 50% of patients with pancreatic cancer presents diabetes. But it is an outstanding challenge for researchers to figure out which is the cause and which is the consequence.
Until now, the most common approach has been to study if diabetes could cause pancreatic cancer. “Our team turned the equation around and, for the first time, we asked the question whether pancreatic cancer could cause diabetes,” explains Núria Malats, senior author of the paper. “Using innovative epidemiological and statistical analysis strategies, we found that pancreatic cancer is the cause of the development of diabetes type 3c in 26% of cases.”
Type 3c, or pancreatogenic, diabetes is characterised by an inflammation of the pancreas that interrupts insulin production. It is estimated to represent around 5-10% of all diabetes cases in Western countries, but currently there are few specific markers for it so that it is often misdiagnosed as diabetes type 2. More precise markers to identify it correctly are required; not only to provide adequate treatment to patients but also because the CNIO now shows that a correct classification is crucial for the early diagnosis of pancreatic cancer.
To conduct the study, the team used data from more than 3,500 persons from PanGenEU, a large European study involving centres from six countries, including Spain, and led by Malats, to analyse the relationship between multiple risk factors and pancreatic cancer.
A factor that defines “high-risk” population that could be applied by the National Health Systems
To be able to confront pancreatic cancer at earlier moments, risk populations must be first defined so that they can be monitored to detect the tumour and act on in its early stages. “Using the information from our study, the national health systems could identify possible as yet undetected pancreatic cancer patients, if the patients, in addition to having type 3c diabetes, also have certain risk factors associated with this cancer, such as being obese or a smoker,” says Malats. “All of these factors would help family doctors better select patients who could benefit from more active monitoring or entering screening programs. Our discovery can be transferred to the National Health Systems as a factor to be taken into account for the early detection of pancreatic cancer.”
The researchers wanted to test if type 2 diabetes could also be connected to this cancer, but in this case, the study was unable to establish a clear causal link. “We have seen that the relationship between pancreatic cancer and type 2 diabetes is very complex, with obesity playing a role, too. Further studies are required to fully understand how the metabolic state is reached in which all these phenomena arise.”
The study was funded by the Spanish Health Research Fund, the Carlos III Health Institute, CIBERONC, the Spanish Thematic Network for Cooperative Research in Cancer, the European Cooperation in Science and Technology, the Italian Association for Cancer Research, Cancer Focus Northern Ireland, and ALF (Sweden).

Reference article
Deciphering the complex interplay between pancreatic cancer, diabetes mellitus subtypes and obesity/BMI through causal inference and mediation analyses. Esther Molina-Montes et al (Gut, 2020). DOI: 10.1136/gutjnl-2019-319990
